Caudal Steroid Injection
Lower back pain is one of the most challenging conditions to treat. Unfortunately, it is also one of the most common. Nearly 80% of adults will face lower back pain at some point in their lives, with an estimated 20% of them experiencing chronic lower back pain. When this occurs, a caudal epidural steroid injection may help. Here’s what you should know about this procedure.
What is a caudal epidural steroid injection?
The caudal space is located at the very end of your tailbone. In this space, nerves branch out to provide sensation and motor activity to your legs and lower back.
Caudal epidural steroid injections are a combination of a steroid and a local anesthetic that is delivered via injection to this space to treat chronic back and lower extremity pain. The steroid reduces inflammation and irritation, while the anesthetic interrupts pain messages to the brain. The medicines spread to the most painful levels of your spine, reducing inflammation and irritation.
With a caudal steroid injection, the injection takes place between the dura (where your spinal fluid is) and the thickest ligament in the caudal vertebra.
What conditions can a caudal epidural steroid injection help with?
Pain that originates from the caudal space typically radiates down the back of your buttocks and into the lower extremities. Some people describe this sensation as pins and needles, while others describe it as pain that is sharp and shooting.
The technical term for this type of pain is sciatica or lumbar radiculitis. Rather than describing a specific condition, this type of pain is characterized by pain, weakness, or sensory changes along the sciatic nerve pathway in the lower back and lower legs. A caudal epidural steroid injection can be helpful for sciatica caused by the following conditions.
Herniated and bulging discs
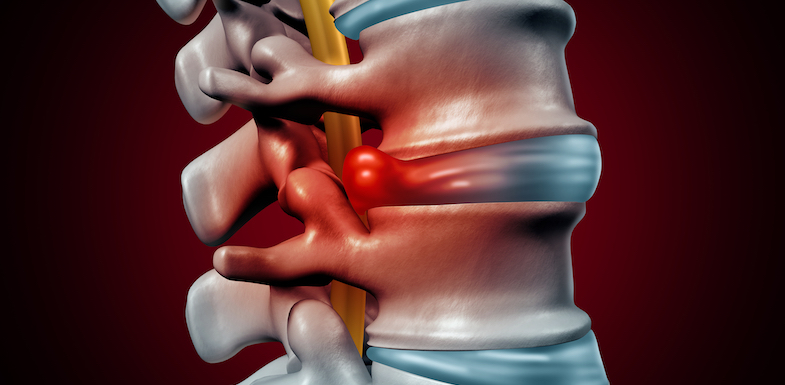
Separating each individual vertebrae are discs that act as cushions that minimize the impact that the spinal column receives. Since the discs are designed to be pliable and provide support, they have a tendency to herniate backwards through the outer ligaments when excessive pressure is applied, causing irritation to adjacent nerves.
Herniated disc is one of the most common causes of chronic lower back pain and sciatica. It accounts for up to 10% of all lower back pain complaints.
Degenerative lumbar spinal stenosis (DLSS)
This disorder occurs due to narrowing of the spinal canal that causes nerve impingement. Spinal stenosis can result in persistent pain in the lower back and lower extremities. Because spinal stenosis is most often due to normal aging and spinal wear and tear, it is the most common reason adults over the age of 65 receive spinal surgery.
For those who suffer from spinal stenosis, they often experience:
- Difficulty walking
- Chronic back and leg pain
- Decreased sensation in the lower extremities
- Decreased physical activity
Many people with spinal stenosis experience sciatic pain on both sides of their body, a condition that makes daily life very challenging.
Commonly, sciatic pain goes into remission with periods of decreased or absent symptoms. When the nerves in the lower back compress without relief, the pain often returns and can lead to a chronic pain syndrome.
An overview of the caudal epidural steroid injection procedure
The procedure for a caudal steroid injection is simple and usually takes less than 15 minutes. You position yourself facedown on the table, and your doctor will prepare the area for injection by cleaning it thoroughly. Most often, you will receive a mild IV sedative to relax you before a local anesthetic is injected into the lower back to numb the area.
Once you are comfortable, your doctor uses fluoroscopic guidance to inject dye into the space to confirm the correct placement for the medication. Once confirmed, medication is injected into the epidural space. This injection includes both a long-lasting steroid and an anesthetic (e.g., lidocaine or bupivacaine).
This procedure may be done in concert with a technique called epidural lysis of adhesions, or the Racz Procedure. This procedure can destroy scar tissue in the epidural space. Scar tissue often results from prolonged irritation, inflammation, or previous surgery in the area.
You can learn more about epidural steroid injections in the following video.
Side effects and risks
Many people do not want to undergo spinal surgery because of the risks associated with it. Caudal epidural steroid injections can help many people avoid spinal surgery.
As with all procedures, though, it does have risks. These are typically rare, but can include the following:
- Bleeding
- Infection
- Headaches
- Nerve damage
The medications also come with pharmacological risks. These risks include:
- Allergic reaction
- High blood sugar
- Decreased immune response
- The potential for weight gain
Along with proper technique, your doctor will reduce your risks by using fluoroscopic guidance to position the needle and watch the medication spread during the procedure.
Recovery
Many patients feel immediate pain relief after this procedure but may find it return after the local anesthetic wears off. This is normal and should not be considered a final result.
On the day of the injection, rest and give yourself the day off. If you experience pain or swelling at the injection site, ask your doctor about over-the-counter anti-inflammatory medications to control this. An ice pack on the injection site can also help ease swelling.
You should be able to resume your normal activities the next day. You should feel pain relief in approximately ten days. If you are still feeling pain at your two-week follow-up, talk to your doctor about your options.
Could a caudal epidural steroid injection help me?
The most important and greatest success achieved with the use of epidural steroid injections is the rapid relief of pain symptoms. This often allows patients to experience enough relief to resume their normal daily activities. It also makes it easier to attend physical therapy to correct the underlying issue.
A study in 2017 found that caudal epidural steroid injection was very successful in the short term management of lower back pain. Another small-scale study in 2018 confirmed that regular caudal epidural steroid injections were consistently effective in managing chronic, intractable lower back pain from any cause.
If your pain has lasted longer than four weeks or is severe in nature, it’s important to see your doctor. Early intervention can decrease the chances of developing a worsening chronic pain syndrome.
References
- Fluroroscopically Guided Caudal Epidural Steroid Injections for Lumbar Spinal Stenosis: A Retrospective Evaluation of Long Term Efficacy. Barre, Lisha. Pain Physician 2004; 7:187-193.
- Rheumatology (Oxford). 2005 Nov;44(11):1399-406. Epub 2005 Jul 19 Arden NK, Price C, Reading I, Stubbing J, Hazelgrove J, Dunne C, Michel M, Rogers P, Cooper C; WEST Study Group. Rheumatology (Oxford). 2005 Nov;44(11): 1399-406. Epub 2005 Jul 19 PMID: 16030082
- Interventional techniques: evidence-based practice guidelines in the management of chronic spinal pain. Boswell MV, Trescot AM, Datta S, Schultz DM, Hansen HC, Abdi S, Sehgal N, Shah RV, Singh V, Benyamin RM, Patel VB, Buenaventura RM, Colson JD, Cordner HJ, Epter RS, Jasper JF, Dunbar EE, Atluri SL, Bowman RC, Deer TR, Swicegood JR, Staats PS, Smith HS, Burton AW, Kloth DS, Giordano J, Manchikanti L; American Society of Interventional Pain Physicians. Pain Physician. 2007 Jan;10(1):7-111 PMID: 17256025