Plantar Fasciitis
Our feet are hardworking and often underappreciated – until it’s too late. With 25% of the bones in the body; 100 ligaments, muscles, and tendons; and more than 30 joints, these weight-bearing workhorses are susceptible to all kinds of pain. One of these sometimes debilitating conditions is plantar fasciitis. Here’s what you should know about preventing and treating this foot pain condition.
What is plantar fasciitis?
The plantar fascia is a thick tendon that connects the heel of the foot with the ball. Offering additional support as it crosses the arch of the foot, the plantar fascia is susceptible to injury and irritation that leads to pain and inflammation. If this tendon becomes torn, compressed, or irritated, a painful condition known as plantar fasciitis occurs.
Plantar fasciitis affects approximately 10% of the adult population of the U.S. It’s the most common form of chronic pain of the heel and foot in adults. If left untreated, plantar fasciitis can lead to bone spurs that require surgical intervention. It can also severely impact your ability to move and function daily.
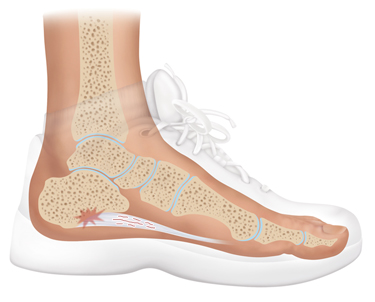
Plantar fasciitis symptoms
Plantar fasciitis symptoms may evolve as you move through your day. People who have plantar fasciitis often limp out of bed first thing in the morning with sharp pain as they first put weight on their feet. When the fascia loosens with use, the pain typically subsides a bit. The first few steps of your day are often the most painful because the fascia is not stretched or used during sleep. Likewise, you may have increased pain after any longer periods of non-activity.
Other plantar fasciitis symptoms include:
- Stiffness on the bottom of the heel
- Ache on the arch of the foot
- Sharp pain or burning when first putting weight on the foot
- Swelling and redness
The pain may be more severe if climbing stairs or performing intense activity. Pain onset may be gradual, or it may be intense and sudden. The severity of your symptoms depends on the level of activity, the amount of damage, and your overall health.
What causes plantar fasciitis?
Plantar fasciitis risk factors are both mechanical and functional.
Overuse and strain are the most common cause of injury to the plantar fascia ligament. Not completing a proper warm-up routine before engaging in physical activity or becoming involved in a new exercise routine after a significant period of time with little to no physical activity can place you at greater risk for developing this condition.
People with arch problems—either too-high arches or flat feet—are also at risk for plantar fasciitis. Wearing shoes without proper arch support can exacerbate arch issues and cause fascia inflammation.
The way a person uses their feet can also cause plantar fasciitis. The fascia can adjust only so far before it is stretched to the point of pain, and certain activities increase your chances of developing plantar fasciitis. Long-distance running, running on uneven surfaces, or a tight Achilles tendon are primary and common causes of inflamed plantar fascia.
It is important to note that bone spurs are not the cause of the fascia pain. These calcium deposits are the foot’s reaction to the inflamed plantar fascia, almost like your feet are trying to protect themselves with additional growth. The spurs are a reaction by the bone to the fascia’s inflammation. Because of this, they often develop together.
Who is most at risk?
Plantar fasciitis is most commonly found in men age 40-70 and is the leading cause of orthopedic care for the feet. Obesity or sudden weight gain also places more pressure on your feet and can cause a sudden onset of symptoms.
There is also some indication that genetics play a role in plantar fasciitis, as those with a first-degree relative with this condition are more susceptible themselves.
People with metabolic issues such as liver diseases and diabetes are also at increased risk. Poor circulation in the feet can lead to irritation in the plantar fascia.
Do I have plantar fasciitis?
To diagnose plantar fasciitis, your doctor will start by asking questions about your pain and health history. They may also take a series of X-rays of your foot. If a bone spur is present, plantar fasciitis is a likely diagnosis. An X-ray can also look for hairpin fractures in the bones around the foot that are also common in those experiencing this type of pain.
Additionally, a thickening and inflammation of the fascia from the ball of the foot to the heel is a common sign of plantar fasciitis.
If no bone spurs are present and other visible signs of plantar fasciitis are not obvious, your physician may ask you to keep a pain journal for a period of time to note when pain occurs and what you are doing. If physical activity is causing stress on the plantar fascia that is not yet visible on an X-ray, they can recommend supportive measures to prevent any further inflammation or irritation.

What plantar fasciitis treatments can help me?
Because this condition can make movement incredibly painful, many sufferers might be tempted to restrict or limit stretching of the bottom of the foot. Unfortunately, this will make the condition worse and harder to treat.
Those with mild cases of plantar fasciitis may typically treat their pain with at-home interventions. Always follow your doctor’s advice for your recovery. Above all else, allow ample time for full recovery. You may not achieve a full recovery for several weeks or even months. Though you may no longer experience symptoms of pain, stiffness, or weakness, the ligament may still not be fully healed.
For best results, try some of the following to relieve symptoms, heal the fascia, and prevent a reoccurrence or worsening of symptoms.
- Rest: In the acute phase, rest and ice may provide the most relief
- Over-the-counter medications: Acetaminophen and ibuprofen reduce inflammation and treat pain without a prescription (but use as directed)
- Stretching: Yoga toe squats and other plantar fasciitis exercises done regularly can help gently exercise and lengthen the tendons, especially in the morning
- Rolling: Use a small hard ball or massage equipment made to release knots to actively roll out the area under your foot
- Athletic tape: Taping the foot for support can relieve symptoms and keep you up and moving around
- Exercises: Strengthening the calves especially can help prevent symptoms from worsening
- Weight loss: By losing weight, you can reduce overall pressure on the foot and markedly improve your symptoms
- Orthotics: Wearing the proper shoes for plantar fasciitis can provide support before, during, and after healing, and night splints can help to gently stretch the foot during rest
- Physical therapy: A focused series of strengthening and stretching exercises can help you reduce your pain
- Cortisone shots: These shots decrease inflammation and pain for sufferers who experience severe plantar fasciitis and can be done in concert with physical therapy
- Surgery: In rare, severe cases, some patients may need to consider surgery for their foot pain
References
- Wapner KL, Parekh SG. Heel pain. In: DeLee JC, Drez D Jr, Miller MD, eds. DeLee and Drez’s Orthopaedic Sports Medicine.3rd ed. Philadelphia, Pa: Saunders Elsevier; 2009:section F.
- Abu-Laban RV, Ho K. Ankle and foot. In: Marx JA, Hockberger RS, Walls RM, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 7th ed. Philadelphia, Pa: Mosby Elsevier; 2009:chap 55.
- Review Date: 2/19/2011.
- Reviewed by: Linda J. Vorvick, MD, Medical Director, MEDEX Northwest Division of Physician Assistant Studies, University of Washington, School of Medicine; C. Benjamin Ma, MD, Assistant Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.