Shingles
If you are an older adult who experienced chickenpox in childhood or was never vaccinated against it, you may be at increased risk for shingles. Here’s what you need to know about its causes, complications, and treatments.
What is shingles?
Shingles is the name for a painful, inflamed rash caused by a viral infection in the nerves.
Also called herpes zoster, shingles is a rash caused by the varicella-zoster virus. This same virus causes chickenpox. For those vaccinated for chickenpox in childhood, shingles is most likely not a concern, but adults who were not vaccinated or who contracted chickenpox as children, the virus remains in their system for life. The inactive virus may remain dormant forever, but up to 25% of adults will experience the painful rash that occurs when the virus reactivates.
There is no clear reason why some people develop this condition and others don’t. Often, adults who suffer one attack are older than 60 and had chickenpox as a child. Another risk factor is a compromised immune system that allows the virus to reactivate.
Many worry that shingles is contagious. If a child is exposed to someone with shingles, he or she may develop chickenpox if unvaccinated. On the other hand, adults who come into contact with someone with shingles will not likely be infected.
What is post herpetic neuralgia?
Sometimes the pain in the area where the shingles occurred may last for months or years after the initial outbreak has healed. This pain is called post herpetic neuralgia. It occurs when the outbreak damages your nerves. Pain ranges from mild to very severe. It is more likely to occur in people over 60 years.
Other complications of shingles may include:
- Another attack of shingles
- Blindness (if it occurs in the eye)
- Deafness
- Infection, including encephalitis or sepsis (blood infection) in people with weakened immune systems
- Bacterial skin infections
- Ramsay Hunt syndrome if it affected the nerves in the face
For otherwise healthy people, complications from the shingles virus are unlikely. Complications most often occur in patients with other health conditions (e.g., compromised immune systems) or those who do not seek prompt medical care.
Do I have shingles?
If you are an older adult reading this, you may be concerned that every rash you experience could be shingles.
This condition has characteristic symptoms, though, that are unlike other types of rashes.
Shingles symptoms
Most healthy people that develop shingles will only experience symptoms for a few weeks and the condition most likely will not return. For others, symptoms may linger for a few months. Shingles attacks come in stages. The preliminary symptoms include tingling and burning before a rash appears. Others report headaches, fever, dizziness, and light sensitivity.
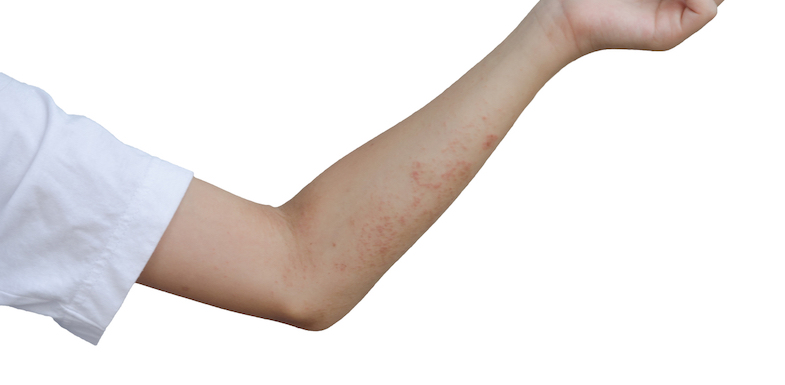
As time progresses, tingling, itching, joint pain, swollen glands, and burning pain commonly develop. The skin rash usually tends to be focused on one side of the body or in one particular location of the body. The rash is often seen on the spine, stomach, and chest, although you may also find outbreaks on the face and mouth.
From there, the rash typically changes to blisters, which burst and create small ulcers. Any scratching can cause the blisters to burst and may possibly scar your skin. Within two to three weeks, the ulcers heal.
Other symptoms include:
- Abdominal pain
- Chills
- Facial distortion due to muscle cramping
- Fever
- Headaches
- Joint pain
- Swollen glands
- Vision issues
In cases where the characteristic rash appears on the face, patients often experience embarrassment or self-consciousness. This is normal, but do remember that all of these symptoms are temporary and should disappear as the rash begins to clear.
Diagnosis
Your doctor can often make a diagnosis by looking at your skin and asking questions about your medical history. If you have a rash accompanied by the above symptoms and also had chickenpox, the diagnosis is usually very clear.
Tests are rarely needed but may include taking a skin sample to see if the skin is infected with the varicella-zoster virus. This is more likely if you did not get vaccinated against chickenpox but do not remember being infected with them.
Blood tests may show an increase in white blood cells and antibodies to the chickenpox virus but cannot confirm that the rash is due to shingles.
If your medical history indicates the possibility of shingles, and the symptoms are present, chances are good that’s your diagnosis.
How to treat shingles
In the majority of cases, herpes zoster clears in two to three weeks and rarely recurs. There is currently no direct cure for shingles, but many types of treatment can decrease your painful symptoms or shorten the duration of the virus. It is important to begin treatment for shingles at the onset of symptoms to reduce the likelihood of complications.
There are a number of different treatment options for more severe or long-lasting cases. Here’s an overview of what your doctor may recommend.
Antiviral medications
Your doctor may prescribe an antiviral medication to fight the virus, if needed. Antivirals help to reduce pain and complications, shortening the outbreak of shingles.
Start antiviral medications within 24 hours of feeling pain or burning and preferably before the blisters appear. The drugs are usually given in pill form. In some cases, antivirals will be most effective when administered intravenously.
Anti-inflammatory medications
Not all people respond well to corticosteroids, and the side effects may not be worth it for more at-risk populations.
Antihistamines
For patients who experience itching, antihistamines (taken by mouth or applied to the skin) can reduce itching.
Over-the-counter pain medicines
Some patients find pain relief with non-steroidal anti-inflammatory drugs like ibuprofen or naproxen sodium.
Zostrix, a cream containing capsaicin (an extract of pepper), may also reduce the risk of post herpetic neuralgia. You can apply it for acute pain relief as well.
Self care
Cool, wet compresses can reduce your pain. Soothing baths and lotions, such as colloidal oatmeal bath, starch baths, or calamine lotion, may help to relieve itching and discomfort.
Complementary and alternative types of therapy, such as yoga and relaxation, may also help with pain relief. These types of therapy help you focus your energy and attention on something other than the painful symptoms.
If a fever is present, rest and take it easy until the fever is under control.
Keep your skin clean and make not to reuse any contaminated items. Wash non-disposable items in boiling water or otherwise disinfect them before reuse. In the stage where shingles lesions are oozing, avoid contact with unvaccinated people or people who have never had chickenpox (especially pregnant women).
If you are caring for a person with shingles, avoid touching the rash and blisters if you have never had chickenpox or the chickenpox vaccine. This occurs most often for parents caring for their children who have contracted chickenpox.
Can I prevent shingles?
There is a shingles vaccination. Older adults who receive the herpes zoster vaccine are less likely to have complications from shingles. Adults older than 60 should receive the herpes zoster vaccine as part of routine medical care.
You may think that shingles is just a complicated rash that will eventually resolve itself, but shingles can lead to serious complications.
Shingles that affects the eye may lead to permanent blindness if you do not receive emergency medical care, and post herpetic neuralgia can lead to ongoing nerve pain. If the virus affects the nerves that control movement (the motor nerves), you may have temporary or permanent weakness or paralysis.
References
- Sampathkumar P, Drage LA, Martin DP. Herpes zoster (shingles) and postherpetic neuralgia. Mayo Clin Proc. 2009 Mar;84(3):274-80. [PubMed]
- Whitley RJ. Varicella-Zoster virus. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2009:chap 137.
- Advisory Committee on Immunization Practices. Recommended adult immunization schedule: United States, 2010. Ann Intern Med. 2010;152:36-39.