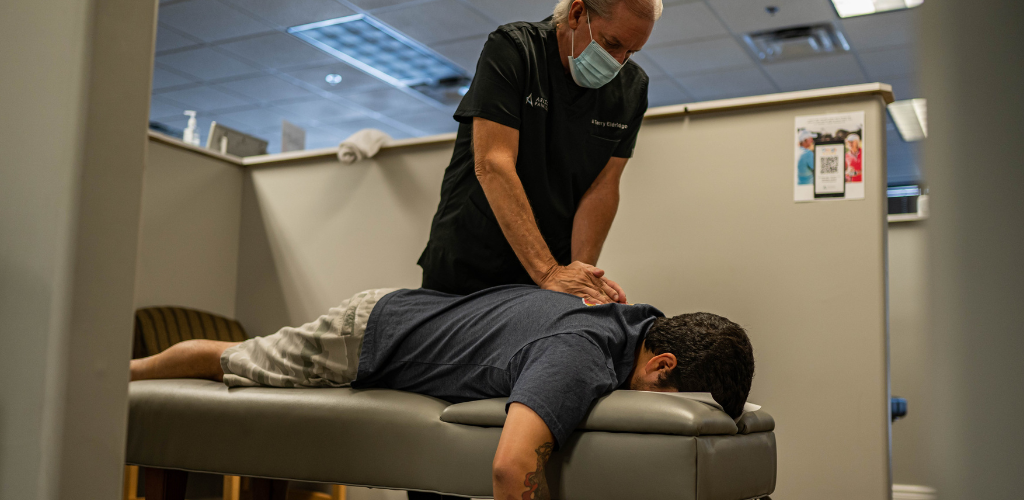
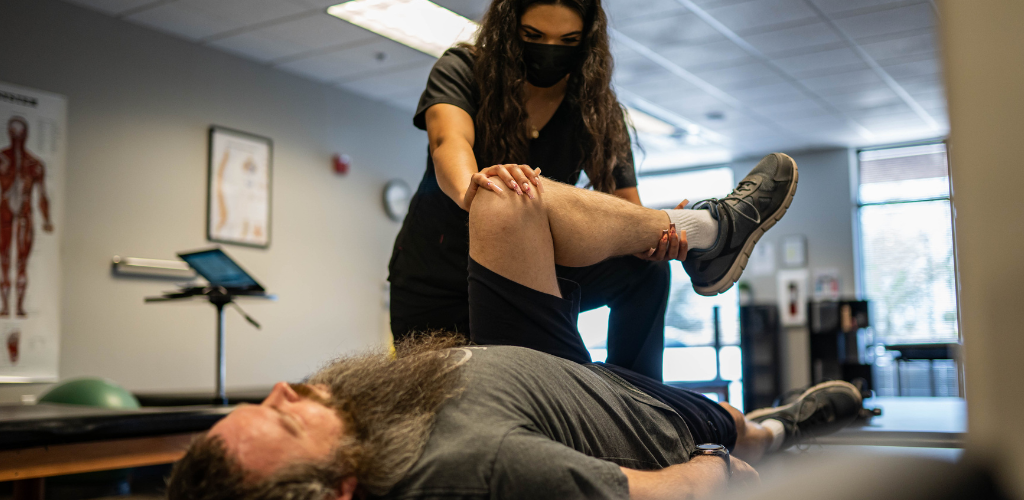
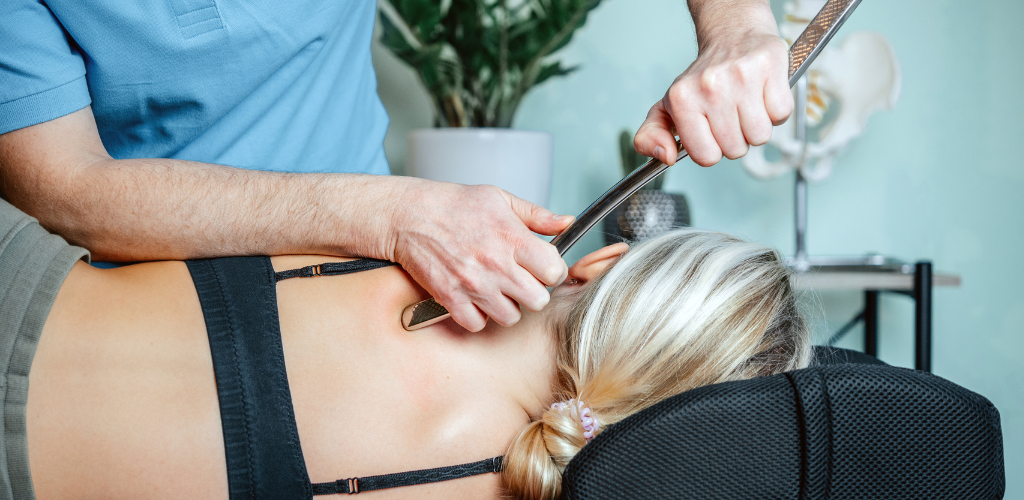
Pain Relief Starts at Our Integrated Pain Clinics.
Our integrated team of chiropractors, advanced pain practitioners, and medical doctors work in-clinic to identify the root cause of your pain and develop a treatment plan that gets you out of pain for good.
Our Integrated Clinical Services
Don’t just live with your pain. Schedule your appointment and let’s get you back to living a life you love.
Top Tier Care Starts with Top Tier Providers.
Our collaborative approach allows for providers of all specialties and expertise to work together to develop and implement a comprehensive treatment plan that gets you out of pain. Get to know each of our providers by clicking their headshots below.
Chiropractors

Dr. Bryan Sims, DC
Chiropractor
Bio

Dr. Mark Frogley, DC
Chiropractor
Bio

Dr. Mitch Healey, DC
Chiropractor
Bio

Dr. Grady Swick, DC
Chiropractor
Bio

Dr. Terry Eldridge, DC
Chiropractor
Bio

Dr. Mike Voisin, DC
Chiropractor
Bio

Dr. Ryan Schulze, DC
Chiropractor
Bio

Dr. Austin Schirck, DC
Chiropractor
Bio

Dr. John Koch, DC
Chiropractor
Bio

Dr. Dave Meyers, DC
Chiropractor
Bio
Advanced Practicing Providers

Amy Martin
Nurse Practitioner
Bio

Jamie Ahner
Physician Assistant
Bio

John Hammonds
Nurse Practitioner
Bio

Elizabeth Colman
Nurse Practitioner
Bio

Maria Salajan
Nurse Practitioner
Bio

Alie Bjelobrkovic
Nurse Practitioner
Bio

Taylor Shin
Physician Assistant
Bio

Katie Wilson
Nurse Practitioner
Bio

Violetta Melkum
Nurse Practitioner
Bio

Keata Bhakta
Nurse Practitioner
Bio

Robin Pond
Physician Assistant
Bio

Paul Morris
Nurse Practitioner
Bio

Elyse Polanco
Nurse Practitioner
Bio

Roberto Ramirez
Nurse Practitioner
Bio

Dominique Dayrit
Nurse Practitioner
Bio
Ready to experience life without pain? Schedule your appointment
Real Success Stories in our Clinic
Contact us to schedule your appointment today.
Pain Conditions
Pain conditions are hard to live with. For those in chronic pain, there may be confusion. You are suffering from back pain, but what causes it? You have been living with chronic daily headaches for months; is it just stress? Or, is your knee pain from an old injury or something else?
At Arizona Pain, we are always working to diagnose the cause of your pain. Your specific pain may come from any number of causes, and it is our life’s work to not only find these causes, but then also to treat them with our interventional procedures, chiropractic care, and behavioral health programs.
Find out what is causing your pain by reviewing information on the most common pain conditions below. Each is explained by our trustworthy, award-winning team at Arizona Pain, noting common symptoms and treatment approaches.
List of Common Pain Conditions
- Post Herpetic Neuralgia
- Post Laminectomy Syndrome
- Prolapsed Disc
- Reflex Sympathetic Dystrophy
- Rotator Cuff Tear
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Shingles
- Shoulder Pain
- Spinal Stenosis
- Tension Headaches
- Trigeminal Neuralgia
- Upper Back Pain
- Vertebral Body Fractures
- Vertebral Compression Fractures
- Whiplash Pain
Don’t just live with your pain. Schedule your appointment and let’s get you to experience life without pain.
Interventional Pain Treatments
Arizona Pain is dedicated to finding the source and cause of your pain and helping you achieve your normal lifestyle that has been lost. We help you get your life back with a variety of pain treatments.
For example, we may recommend that you undergo a minimally invasive, non-surgical procedure in our state-of-the-art, on-site procedure center. These treatments are on the cutting-edge of pain management and have all been shown to be extremely successful in treating pain. All procedures are outpatient procedures. This means you’ll be able to go home that day. Many of the treatments we perform show instant results and are able to help our patients reclaim their lives.
List of Offered Pain Treatments
Contact us to find which of our treatments may be a fit for you.
Diagnostic Procedures
Too often, pain patients have heard the pain “is all in your head.” Unfortunately, this leads to frequent misdiagnosis or underdiagnosing of pain conditions. We know the pain you experience is real.
At Arizona Pain, we work with patients to uncover their diagnosis from the start. This forms the foundation of care as we build your individualized pain treatment plan. Some of the tests and studies we perform may include the following.
List of Offered Diagnostic Procedures
- Electromyograms (EMG)
- MRIs
- X-Rays
- CT Scans
- Full Neurological Examinations
Meet our Pain Providers
Medical
Doctors
Our double-board certified pain doctors help treat pain issues with innovative options.
Advanced Practicing Providers
Our clinicians develop a comprehensive care plan tailored specifically to your diagnosis.
Chiropractors
Our chiropractors use effective and safe techniques in order to treat pain in their patients.