Radiofrequency Ablation
In the early part of the 20th century, trigeminal neuralgia was a mysterious and incredibly painful nerve disorder that caused excruciating facial pain. After trying many different techniques for pain relief, doctors discovered what seemed to be a miracle: a safe, effective, minimally invasive procedure that relieved the pain of trigeminal neuralgia with few, if any, risks or side effects. Since then, radiofrequency ablation has provided pain relief to people across the globe. Here’s what you should know about this procedure, its benefits, and recovery.
What is radiofrequency ablation?
Radiofrequency ablation was first used in 1931 to treat a patient with trigeminal neuralgia and is now used to effectively treat a variety of chronic pain conditions.
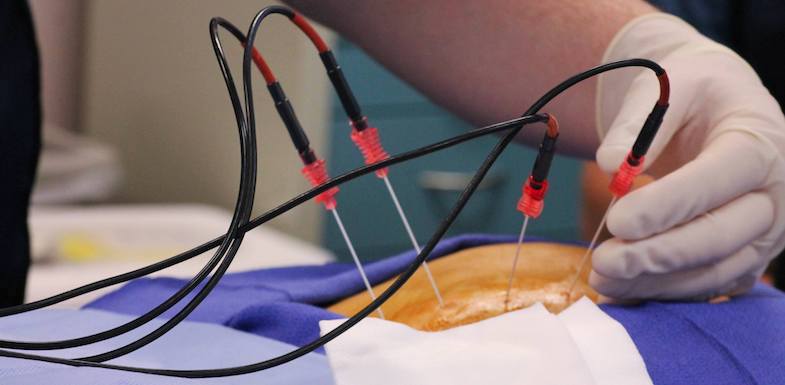
Often used in conjunction with a medial branch block to identify the exact source of nerve pain, radiofrequency ablation (RFA) uses specialized electrodes to disrupt nerve conduction. A probe is inserted through a needle, and controlled delivery of heat is placed along the nerve sending pain signals. This pain relief technique can help with:
Radiofrequency ablation is a minimally-invasive procedure that can help patients with chronic pain to avoid surgeries and long recovery times.
There are two main types, including:
- Radiofrequency thermo-coagulation
- Pulsed radiofrequency
Radiofrequency thermo-coagulation
With this form of the procedure, an electrode is heated to 50-80°C and kept at that temperature for several minutes.
Electro-thermal heat is generated, which allows for destruction of surrounding pain fibers, thereby decreasing your pain. This is also sometimes referred to as continuous radiofrequency ablation.
Pulsed radiofrequency
This technique is similar to continuous radiofrequency ablation but uses a lower level of heat to stun the nerve instead of destroying it. This heat is also delivered in pulses.
The type used depends on the desired outcome and the type of pain (or other condition) you’re suffering from.
How does radiofrequency ablation work?
Regardless of which type is most effective in treating your pain, they both act on the spinal nerves in the same way.
The individual vertebrae (bones of the spine) provide a flexible support structure while also protecting the spinal cord. The facet joints of the spine are a moveable connection that links one vertebra to another. Facets are innervated by the medial branch nerve, which provides sensation to the joint. Medial branch nerves are small nerve branches that communicate pain from the facet joints to the brain.
The complex structure of the vertebrae and its intertwining with the nerves of the spinal cord means that any damage, injury, or condition that affects the spine has the potential to affect the nerves. Radiofrequency ablation starts with a medial branch block that locates the exact nerve affected so that pain signals can be blocked.
How can radiofrequency ablation help me?
Radiofrequency ablation helps with a variety of conditions that include chronic pain conditions as well as other conditions that lead to pain. These include:
- Peripheral neuropathies
- Sympathetically mediated pain
- Complex regional pain syndrome
- Headaches
- Neck and back pain
- Stroke-related pain
- Disc denervation
Radiofrequency ablation is used to treat pain syndromes most often, but is also used for the following:
- Cancer tumors
- Cardiac arrhythmia
- Dermatology
- Barrett’s esophagus
- Varicose veins
- Obstructive sleep apnea
Radiofrequency ablation benefits
In a clinical research study for patients treated with radiofrequency therapy, 21% had complete pain relief, and 65% reported mild to moderate pain relief. The majority of the respondents reported reduction in the use of pain medications. None of the patients developed significant infection, bleeding, hematoma formation, or numbness as complications to their therapy.
Radiofrequency ablation is an extremely safe, well-tolerated method selected to treat many causes of chronic pain. If your pain responds well to an initial treatment, a follow-up treatment may be helpful. As a non-invasive therapy for lower back pain, radiofrequency ablation helps to increase mobility, ease pain, and reduce the use of analgesics.
In a 2012 study, pulsed radiofrequency showed excellent pain relief for more than 80% of the patients. These same patients had positive outcomes at two, six, and 12 months (although pain relief percentages were slightly lower over time). Since pulsed radiofrequency does not completely destroy the nerve, a return in pain is to be expected as the nerves regenerate, and the treatment can be repeated.
Contraindications
Although many people have good pain-relieving results with this procedure, radiofrequency ablation is not for everyone.
Patients with the following conditions may not be good candidates for radiofrequency ablation:
- Active cold or infection
- Pregnancy
- Uncontrolled diabetes
- Issue with blood clots
- Use of steroids
- Weight of 250 pounds or more
All of these conditions increase your risk of complications. Talk to your doctor to discuss all of your options and potential risks.
What should I expect for the radiofrequency ablation procedure?
Radiofrequency ablation is an outpatient procedure performed with a local anesthetic. If you are nervous about the procedure, your doctor may decide to use a mild general anesthetic in addition to a local numbing medicine. This can help you stay calm, still, and relaxed during your procedure.
Prepare yourself before the procedure by talking to your doctor about any medications you are taking and getting answers to your questions. Even though the procedure uses local anesthesia, you will need someone to drive you home afterwards.
Your doctor will clean and sterilize the area along the spine where the procedure will be performed. They may use a topical anesthetic to numb your skin before administering a local anesthetic. This procedure should be completely pain free, but you may feel a prick and a sting with the first injection of anesthetic. If you are still uncomfortable, let your doctor know.
Once you are comfortable, they’ll place another needle. Using fluoroscopic guidance, your doctor moves a needle into the area for the radiofrequency ablation procedure. A small microelectrode travels through the needle to rest near the targeted nerve tissue.
A mild electrical current is delivered through the microelectrode to make sure the correct nerve is targeted. If the microelectrode is in the proper place, a numbing agent is applied to the nerve before a heat-generating electrical current is delivered. Corticosteroids may also be used if there is inflammation present.
The entire procedure takes between 30 and 90 minutes, with the entire appointment being no more than a few hours long. You should be comfortable and pain free the entire time. If you do feel pain, it could mean that you need more numbing medication or the proper nerve was not targeted, so let your doctor know.
Radiofrequency ablation recovery
After the procedure, take the remainder of the day to rest and recover. You may feel slightly sore at the injection site. You can treat this pain with over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs). Ice packs can help with any swelling you experience, as well.
For 48 hours, avoid strenuous exercise and heavy lifting. Operating heavy machinery or driving is not recommended, and do not enter water (for swimming or bathing). As you recover, you can gradually return to regular levels of activity. This is not major surgery, and your recovery time should be swift and relatively easy.
Most patients experience pain relief that lasts for months, but you can also repeat it if, after three weeks, your pain persists. Your pain relief should generally last for six months or more. You can repeat this procedure if necessary for continued pain relief.
You may experience mild soreness in the injection site for up to two weeks, but it should not be as painful as the condition for which you are being treated. If soreness persists, talk to your doctor.
Radiofrequency ablation side effects and risks
As with any medical procedure, there are risks and potential complications. Although complications rarely occur, it’s important to understand the risks with radiofrequency ablation. In general, these risks are low and complications are rare.
Potential radiofrequency side effects and risks include:
- Bleeding
- Infection
- Worsening of pain symptoms
- Discomfort at the point of injection
In very rare cases, patients may experience motor nerve damage, paralysis, muscle weakness, and severe pain. Talk to your doctor about your specific risk factors for these more severe side effects.
If you experience swelling, excessive pain, and/or fever, contact your doctor immediately. These could be signs of a potentially dangerous infection.
References
- Radiofrequency ablation in the management of spinal pain Menno E. Sluijter MD, PhD Institute for Anesthesiology and Pain Treatment, Swiss Paraplegic Center, Nottwil, Switzerland Lord SM, Bogduk N.
- Radiofrequency procedures in chronic pain. Best Pract Res Clin Anaesthesiol. 2002 Dec;16(4):597- 617.
- Clinical significance of trigeminal neuralgia treated using radiofrequency thermocoagulation (RFT) with different approaches Chen Z, Zhao Z, Li M, Yang Y. Hua Xi Kou Qiang Yi Xue Za Zhi. 2001 Aug;19(4):240-2.
- Radiofrequency-thermocoagulation in the treatment of trigeminal neuralgia: analysis of 100 cases Motta P, de Souza MT, Sengupta RP. Arq Neuropsiquiatr. 1980 Mar;38(1):33-44
- Radiofrequency thermocoagulation of Gasserian ganglion and its rootlets for trigeminal neuralgia.Sengupta RP, Stunden RJ. Br Med J. Jan 15;1(6054):142-3.
- A systematic review of therapeutic facet joint interventions in chronic spinal pain. Boswell MV, Colson JD, Sehgal N, Dunbar EE, Epter R. Pain Physician. 2007 Jan;10(1):229-53.
- Radiofrequency neurotomy for lumbar pain. Murtagh J, Foerster V. Issues Emerg Health Technol. 2006 May;(83):1-4
- Sphenopalatine ganglion pulsed radiofrequency treatment in 30 patients suffering from chronic face and head pain. Bayer E, Racz GB, Miles D, Heavner J. Pain Pract. 2005 Sep;5(3):223-7