Sphenopalatine Ganglion Block
Facial pain and pain that occurs due to cluster headaches and migraines can be debilitating. For those who suffer from certain types of facial pain the risk of suicide actually increases. Sphenopalatine ganglion block is a procedure that may help ease or relieve the pain, with few side effects and long-lasting results. Here’s what you should know about this pain management approach.
What is a sphenopalatine ganglion block?
A sphenopalatine ganglion block is a short, minimally-invasive procedure that is effective at treating some types of acute and chronic facial and head pain. How it works comes down to your anatomy.
The sphenopalatine ganglion is a bundle of nerves located below the nose, within the slight depression in the skull on either side of the nose called the pterygopalatine fossa bone cavity. This ganglion is linked to the sensory, parasympathetic, and sympathetic nervous systems, all of which are transmitters and receivers of pain signals.
The sphenopalatine ganglion sends nerve fibers to the lacrimal gland, glands of the nasal cavity, paranasal sinuses, palate, and upper pharynx.
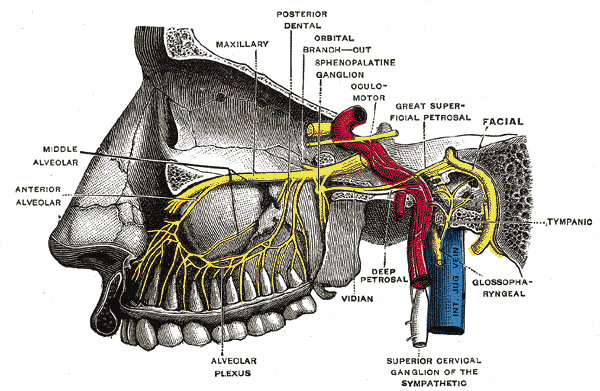
Other important markers pass through the ganglion, including the trigeminal nerve, responsible for enervating the head and face. This bundle of nerves has been the primary target of treatment for the relief of headache pain for over a century, as it is directly affected by a variety of stimuli that seem to trigger head pain.
In addition to the trigeminal nerves, other important fibers also pass through and are affected by the sphenopalatine ganglion. These include:
- Postganglionic parasympathetic fibers: These transmit messages to certain muscles
- Somatic sensory afferents: Fibers in the spinal nerves
The signals from all of these can be inhibited by performing a sphenopalatine block. By doing this, you can prevent or completely stop some forms of pain from occurring.
What conditions can sphenopalatine ganglion block help with?
A sphenopalatine ganglion block can treat:
- Migraines
- Cluster headaches
- Other forms of intractable and difficult-to-treat facial pain, most specifically trigeminal neuralgia
The research: sphenopalatine block for migraine and cluster headache
In 2018, researchers found that not only does pain relief come quickly with sphenopalatine ganglion block (about 15 minutes for nearly 71% of patients), but it is also long-lasting. Fifty-five patients received transnasal lidocaine and reported remaining headache-free after two hours (78.4%) and 24 hours (70.4%). The patients who were not completely headache-free experienced a significant reduction in pain that lasted as long as those who had no pain at all.
This 2018 study simply confirmed what a review of studies found a year earlier: not only does sphenopalatine block work to relieve migraine and cluster headaches, but it is minimally invasive and comes with few (if any) lingering side effects.
This review also noted that a sphenopalatine block followed by radiofrequency ablation to more permanently disrupt the nerve signal brought about the best, long-lasting results with few side effects or risks.
The research: sphenopalatine block for head and neck pain related to cancer
In research that brings great relief not only to cancer patients but also their families and caregivers, another study in 2017 found that sphenopalatine ganglion block delivered transnasally at home was effective in relieving cancer pain in the head and neck even when opioids and other prescription pain medications were not.
The research: trigeminal neuralgia
For trigeminal neuralgia sufferers, pain relief may seem impossible. This condition is often perplexing and hard to treat, given that it can be hard to diagnose a root cause to address.
No matter what the cause, small-scale studies are showing that trigeminal neuralgia patients are experiencing profound relief with sphenopalatine ganglion blocks, nearly instantly and for long periods of time.
An overview of the sphenopalatine ganglion block procedure
Covered by a layer of connective tissue and mucous membrane, the sphenopalatine ganglion can be accessed for treatment with either a topical application or an injection of medication.
Depending on whether your doctor performs this block topically or via injection, this procedure may take anywhere from 15 minutes to 30 minutes at most. If you are anxious or in pain, your doctor can provide intravenous sedation to make your procedure more comfortable. You can watch an overview of this procedure in the following video.
The three most common approaches for the sphenopalatine ganglion block, include:
- Transnasal
- Transoral
- Lateral
Let’s look at each of these approaches in more detail.
Transnasal
The transnasal approach is the simplest and most common technique among the three. You will lie down on your back and extend your neck. Then, you open your nose as if you are going to take a big sniff.
Your doctor will look at your nostrils for any visible polyps, tumors, or significant septal deviation before beginning. This procedure is performed with a local anesthetic (lidocaine) that is placed onto the nostril so you can briskly inhale it to numb the area.
This draws the local anesthetic towards the back of your nose, lubricating it and anesthetizing it in the process to make the procedure more comfortable.
Remember that the sphenopalatine ganglion block can be performed either topically or by injection. If your doctor decides that a topical application is best, they will introduce a sterile cotton tipped applicator dipped in anesthetic, slowly moving it along the wall of the inside of the nose until it reaches your nasopharynx (the place where your nasal cavity and soft palate meet at the upper area of the pharynx).
The applicator is usually left in place for approximately 20 to 30 minutes.
Transoral
With a transoral sphenopalatine ganglion block, the general area is flooded.
This approach can help when other points of access are restricted or otherwise inaccessible. Dentists most often perform this type of sphenopalatine ganglion block.
Lateral
Also referred to as the percutaneous infrazygomatic approach, this is a targeted way to deliver the block in a specific space (instead of flooding the area, as in the transoral approach).
If your doctor decides to perform the sphenopalatine ganglion block via injection, they will anesthetize part of your cheek. Next, they will advance a small needle under X-ray guidance through anesthetized tissue to the correct location. After the position is confirmed under fluoroscopy, anesthetic is injected into the ganglion.
Benefits
No matter whether placed topically or via injection, a successful block is marked by profound pain relief.
For patients who have a documented response to administration of local anesthetic onto the sphenopalatine ganglion, you and your physician may decide to perform a neurolysis or radiofrequency ablation of the sphenopalatine ganglion for pain management.
Side effects
The risk for this procedure is very low. The most common side effects of a sphenopalatine ganglion block include:
- Developing a bitter taste in your mouth from the local anesthetic potentially dripping down the back of your throat
- A slight numbness in the back of the throat from the local anesthetic doing the same thing
Both of these side effects pass quickly and are not a cause for concern. Occasionally, some patients may develop a nose bleed from an accidental abrasion inside the nostril. Again, this is a minor side effect.
When dealing with the sinus and nasal cavities, some patients may also experience slight lightheadedness that usually subsides within 20 or 30 minutes after the procedure.
As always, with any procedure that involves local anesthetic, there is a risk of drug allergy and seizure (if the medication is injected into a blood vessel). Tell your doctor if you have had trouble with anesthetic in the past.
Finally, with any penetration of skin and soft tissues, the risk of infection exists.
Recovery
Recovery is nearly immediate after this procedure. If you experience a bitter taste or numbness in the throat, it is helpful to wait until that wears off before eating or drinking anything.
If you received general anesthesia for the procedure, you will need someone to drive you home and should plan to take it easy for the rest of the day.
Note that if pain gets significantly worse; you notice bleeding, redness, or swelling in the injection area; or you start to have a fever, call your doctor, as this could be a sign of infection.
The benefits of this block can be temporary for some people, and the amount and duration of pain relief can vary from person to person. Some may have relief for weeks where others can benefit from the block for years.

Could a sphenopalatine ganglion block help me?
Even with its low-risk (and potentially high reward), sphenopalatine ganglion block is not suitable for every condition. The most common pain conditions treated with this procedure include:
- Acute and cluster headaches
- Trigeminal neuralgia
- Temporomandibular joint (TMJ) pain
- Herpes zoster
- Sluder’s neuralgia
- Paroxysmal hemicrania
- Atypical facial pain
- Head and neck cancer
- Complex regional pain syndrome (CRPS)
- Reflex sympathetic dystrophy (RSD)
- Vasomotor rhinitis
- Pre- and post-operative anesthesia in oral and maxillofacial surgery
There are some conditions for which this type of block has not proven effective. Myofascial facial pain and pain due to fibromyalgia did not respond with pain relief in a way that was statistically significant when compared to placebo.
References
- Ferrante FM, Kaufman AG, Dunbar SA, Cain CF, Cherukuri S. Sphenopalatine ganglion block for the treatment of myofascial pain of the head, neck, and shoulders. Reg Anesth Pain Med. 1998 Jan-Feb;23(1):30-6.
- Janzen VD, Scudds R. Sphenopalatine blocks in the treatment of pain in fibromyalgia and myofascial pain syndrome. Laryngoscope. 1997 Oct;107(10):1420-2.
- Manahan AP, Malesker MA, Malone PM. Sphenopalatine ganglion block relieves symptoms of trigeminal neuralgia: a case report. Nebr Med J. 1996 Sep;81(9):306-9.
- Morelli N, Mancuso M, Felisati G, Lozza P, Maccari A, Cafforio G, Gori S, Murri L, Guidetti D. Does sphenopalatine endoscopic ganglion block have an effect in paroxysmal hemicrania? A case report. Cephalalgia. 2009 May 5.
- Narouze S, Kapural L, Casanova J, Mekhail N. Sphenopalatine ganglion radiofrequency ablation for the management of chronic cluster headache. Headache. 2009 Apr;49(4):571-7. Epub 2008 Sep 9.
- Olszewska-Ziaber A, Ziaber J, Rysz J. [Atypical facial pains–sluder’s neuralgia–local treatment of the sphenopalatine ganglion with phenol–case report] Otolaryngol Pol. 2007;61(3):319-21. [Article in Polish]
- Peterson JN, Schames J, Schames M, King E. Sphenopalatine ganglion block: a safe and easy method for the management of orofacial pain. Cranio. 1995 Jul;13(3):177-81.
- Prasanna A, Murthy PS. Vasomotor rhinitis and sphenopalatine ganglion block. J Pain Symptom Manage. 1997 Jun;13(6):332-8.
- Quevedo JP, Purgavie K, Platt H, Strax TE. Complex regional pain syndrome involving the lower extremity: a report of 2 cases of sphenopalatine block as a treatment option. Arch Phys Med Rehabil. 2005 Feb;86(2):335-7.
- Raj P, Lou L, Erdine S et al. Radiographic imaging for regional anesthesia and pain management. New York, Churchill Living-stone, 2003, pp 66-71.
- Robiony M, Demitri V, Costa F, Politi M. [Percutaneous maxillary nerve block anesthesia in maxillofacial surgery] Minerva Stomatol. 1999 Jan-Feb;48(1-2):9-14. Italian.
- Saberski L, Ahmad M, Wiske P. Sphenopalatine ganglion block for treatment of sinus arrest in postherpetic neuralgia. Headache. 1999 Jan;39(1):42-4.
- Sanders M, Zuurmond WW. Efficacy of sphenopalatine ganglion blockade in 66 patients suffering from cluster headache: a 12- to 70-month follow-up evaluation. J Neurosurg. 1997 Dec;87(6):876-80.
- Stechison MT, Brogan M. Transfacial transpterygomaxillary access to foramen rotundum, sphenopalatine ganglion, and the maxillary nerve in the management of atypical facial pain. Skull Base Surg. 1994;4(1):15-20.
- Varghese BT, Koshy RC. Endoscopic transnasal neurolytic sphenopalatine ganglion block for head and neck cancer pain. J Laryngol Otol. 2001 May;115(5):385-7.
- Waldman S. Atlas of Interventional Pain Management. Philadelphia, WB Sanders, 1998, pp 10-12.
- Waldman, S. Sphenopalatine ganglion block- 80 years later. Reg Anesth 1993; 18:274-276.
- Waxman, S. Correlative Neuroanatomy, 23rd ed. Stamford, Appleton & Lange, 1996. Pp 265-266.
- Windsor RE, Jahnke S. Sphenopalatine ganglion blockade: a review and proposed modification of the transnasal technique. Pain Physician. 2004 Apr;7(2):283-6.
- Windsor R, Gore H, Merson M: Interventional sympathetic blockade. In Lennard T (ed.) Pain Procedures in Clinical Practice, 2nd ed. Philadelphia, Hanley & Belfus, 2000, pp 321-324.
- Yang Y, Oraee S. A novel approach to transnasal sphenopalatine ganglion injection. Pain Physician. 2006 Apr;9(2):131-4.