Trigger Point Injections
When considering chronic pain, it can be tempting to look at a certain joint or group of muscles as the culprit. Sometimes, though, pain originates in one place and then flares up all over the body. When this occurs, trigger point injections can help. This is what you should know.
What are trigger point injections?
Our muscles and organs are completely encased in a thin web of connective tissue called fascia. When the fascia becomes tight or constricted, it can cause pain in the immediate area, but it can also cause referred pain in another area as the body compensates for its restricted movement. Points of tightness, tenderness, or discomfort in a specific muscle or area of the fascia may affect movement, normal function, or the quality of life of people affected by them.
A trigger point injection injects medication directly into those tight areas within muscles or fascia that are causing pain.
These targeted areas for injection are known as trigger points. In some cases, trigger points may be felt under the skin as a knot or nodule. Knots may react with muscle twitches or pain when pressed on with a finger.
The most common medications injected into these points to relieve pain are the local anesthetics lidocaine or procaine.
These injections are an effective treatment for pain or discomfort emanating from a trigger point.
What conditions can trigger joint injections help with?
One of the most common conditions helped by trigger point injections is myofascial pain syndrome. When tightened bands of muscle tissue create abnormal contractions and intensify or spread over time to form small, localized areas within the muscle, these trigger points may indicate myofascial pain syndrome.
Myofascial pain syndrome can contribute to other musculoskeletal disorders such as rotator cuff disease (a condition affecting the upper arm and shoulder) by increasing the strain or pressure on a muscle or muscle group.
The exact mechanism by which myofascial pain syndrome arises and develops has not yet been established. There may be a variety of factors that contribute to this disorder, including damage to or diseases of the fascia or connective tissue.
Autoimmune conditions, in which the body’s own immune system attacks the fascia, may also be factors in myofascial pain syndrome development.
Both cancer and its treatment (e.g. surgery or chemotherapy) can result in damage to healthy fascia or muscles near a tumor, leaving damaged and tightened muscle tissue as a consequence.
The formation of trigger points may also be associated with a range of factors and other conditions. These include:
- Abrupt overload or strain on the affected muscle(s)
- Arthritis
- Decreases in the temperature of the affected muscle(s)
- Emotional distress
- Fibromyalgia
- Gall bladder diseases
- Lumbrosacral radiculopathy (nerve damage in the back) leading to excessive tension in back muscles
- Muscular fatigue
- Muscular trauma
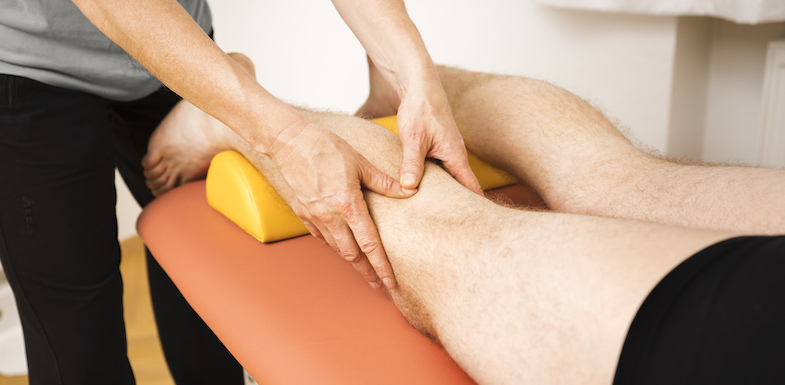
An overview of the trigger joint injections procedure
A trigger point injection procedure is performed on an outpatient basis right in your doctor’s office (or other similar facility).
You will sit or lie in a position that makes the trigger point accessible to your pain specialist. Trigger points are most accurately located and visualized using ultrasound.
Your doctor will clean the skin above this area. They may also apply a topical anesthetic if necessary to minimize your discomfort. Then, the trigger point injection is delivered directly to the affected muscle or area.
In some cases, you may receive multiple trigger point injections in the same area. This ensures complete coverage and thorough deactivation of the trigger point. The average trigger point injection procedure, from start to finish, lasts less than an hour.
Side effects and risks
Trigger point injections are a minimally invasive and safe procedure, but, as with all medical procedures, there are some risks.
Trigger point injections can cause initial reactions such as sudden pain or muscular spasms. However, these reactions are temporary and do not occur in every injection.
Common side effects afterwards may include bleeding or infection in the skin or surrounding tissues. You can minimize these risks by keeping the area clean and bandaged after your procedure.
If you suffer from blood clotting disorders or take medications to reduce clotting, you may not be a suitable candidate for trigger point injections due to the risk of excessive blood loss. These injections may also be unsuitable for pregnant women and those with increased body mass (which may make it challenging to effectively target certain muscles).
The injected anesthetic medications are associated with adverse effects that could also include:
- Numbness or discomfort in the chest
- Temporary headache
- Sensory issues
To minimize your risks, discuss all of your current health conditions, known allergies, and concerns with your doctor beforehand.
Recovery
Follow your doctor’s guidelines because they know your unique health profile. After the procedure, though, you should generally not strain or over-use the treated area for 24 hours.
After 24 hours, your doctor may advise light exercise or stretching of the area. This can help to relax and release the tension and lead to a better result.
Could trigger point injections help me?
In conditions such as fibromyalgia, radiculopathy, and myofascial pain syndrome, trigger point injections may effectively relieve both muscle tension and the pain from these conditions. These injections are especially effective when combined with other treatment modalities (e.g., stretching, light exercise, and acupuncture).
An interesting and relatively new application of trigger point injection is in treating certain types of headache. Trigger points in some muscles of the skull or neck may lead to pain relief for some types of headache pain.
Trigger point injections are a relatively quick and convenient procedure that can help you avoid more extensive surgeries or interventions. For many, they provide another option towards greater pain relief.
References
- CADTH Rapid Response Reports. Botulinum Toxin A for Myofascial Pain Syndrome: A Review of the Clinical Effectiveness. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health. Copyright (c) 2014 Canadian Agency for Drugs and Technologies in Health.; 2014.
- Morjaria JB, Lakshminarayana UB, Liu-Shiu-Cheong P, Kastelik JA. Pneumothorax: a tale of pain or spontaneity. Therapeutic advances in chronic disease. 2014;5(6):269-273.
- Soares A, Andriolo RB, Atallah AN, da Silva EM. Botulinum toxin for myofascial pain syndromes in adults. The Cochrane database of systematic reviews. 2014;7:Cd007533.
- Robbins MS, Kuruvilla D, Blumenfeld A, et al. Trigger point injections for headache disorders: expert consensus methodology and narrative review. Headache. 2014;54(9):1441-1459.
- Suh MR, Chang WH, Choi HS, Lee SC. Ultrasound-guided myofascial trigger point injection into brachialis muscle for rotator cuff disease patients with upper arm pain: a pilot study. Annals of rehabilitation medicine. 2014;38(5):673-681.
- Cardoso LR, Rizzo CC, de Oliveira CZ, Dos Santos CR, Carvalho AL. Myofascial pain syndrome after head and neck cancer treatment: Prevalence, risk factors, and influence on quality of life. Head & neck. 2014.
- Saeidian SR, Pipelzadeh MR, Rasras S, Zeinali M. Effect of trigger point injection on lumbosacral radiculopathy source. Anesthesiology and pain medicine. 2014;4(4):e15500.
- Affaitati G, Costantini R, Fabrizio A, Lapenna D, Tafuri E, Giamberardino MA. Effects of treatment of peripheral pain generators in fibromyalgia patients. European journal of pain (London, England). 2011;15(1):61-69.
- Fernandez-de-Las-Penas C, Cuadrado ML, Pareja JA. Myofascial trigger points, neck mobility, and forward head posture in episodic tension-type headache. Headache. 2007;47(5):662-672.