
If you suffer from back pain, you already know what a negative impact it can have on your life. Activities you once enjoyed and performed with ease suddenly become difficult, and even just trying to sit and relax can be painful. One of the culprits behind many people’s back pain is a herniated disc. Read on to learn more about the common signs, symptoms, and treatments of a herniated disc.
What is a herniated disc?
People sometimes refer to herniated discs as ruptured discs, slipped discs, or disc prolapses. All of these names imply that something has gone wrong with part of your body. But what exactly is a disc, and what happens to it when it herniates?
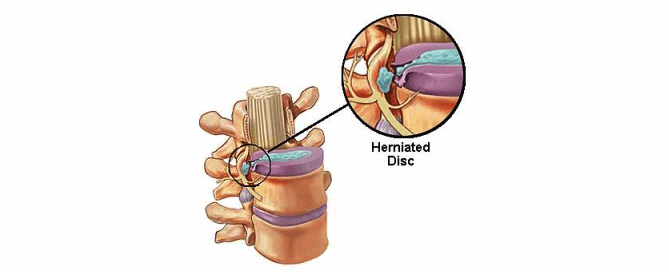
The bones that make up your spine are called vertebrae. They are separated from one another by thin layers, or discs, filled with a jelly-like substance called the nucleus pulposus. In a healthy spine, these discs prevent your vertebrae from grinding against each other, allowing you to move about pain-free.
But, as with all other body parts, these discs can become damaged or broken over time. Sometimes, the outer layer of the disc (called the annulus fibrosus) breaks. This causes the jelly to spill out and forces the vertebrae into direct contact with each other. The jelly may also come into contact with one of the many nerves running up and down the spine.
This can lead to back pain and other uncomfortable, even debilitating symptoms.
Herniated disc vs. bulging disc
Herniation is not the only condition that can affect your spinal discs. A bulging disc occurs when the disc slips from its proper place between the vertebrae. This condition may be completely asymptomatic, or it may cause many of the same problems as a herniated disc, including pain, tingling, and numbness.
The critical difference is that, in cases of a bulging disc, the disc remains intact even as it moves where it isn’t supposed to be. A herniated disc has been damaged in such a way that it is no longer in one whole, undamaged piece. If a bulging disc is left untreated for too long, it may become herniated.
Types of herniated discs
The type of herniated disc you have depends on where it is located. Your back consists of four to five regions, depending on how you divide up the spine.
- Cervical: This refers to the vertebrae in your neck.
- Thoracic: This region covers your upper and middle back, from the base of your neck to approximately just below the ribcage.
- Lumbar: The lumbar region is more commonly referred to as your lower back.
- Sacral: The sacrum is at the base of your spine and consists of several fused vertebrae within your pelvic cavity.
- Coccygeal: Also called the tailbone, the coccygeal region is the very end of your spine. It is sometimes combined with the sacral region rather than split into its own distinct region.
Lumbar disc herniation is the most common type of disc herniation. However, it is possible to suffer disc herniation in the cervical and thoracic regions as well.
What are herniated disc causes and risk factors?
Pretty much anyone can herniate a disc if they are unlucky enough. However, there are certain factors that increase your chances of developing this condition.
Here are some of the most common herniated disc causes and risk factors.
Injury
Herniated disc causes often involve some sort of trauma to your back. This can be something as serious as a fall or sports-related injury, or something as simple as changing positions too abruptly.
The more you put strain on your back, the more likely you are to suffer a herniated disc. This means that athletes and people with physically strenuous occupations are at greater risk than others.
Gender
While herniation can affect people of all genders, males are generally more susceptible to it than females.
Age
As you get older, your bones become more susceptible to injury. This is in addition to the wear and tear that accumulates naturally over a lifetime.
So, while herniated discs can affect people of all ages, they are more likely to occur in people with older, typically more damaged spines.
Lifestyle
Regular exercise is an important part of living a long, healthy life. Without it, your body becomes weaker, making it more likely for something to go wrong.
Being overweight is another risk factor for disc herniation. Extra weight causes the spine to work harder to move your body, and that strain can leave you susceptible to a herniated disc.
What are common herniated disc symptoms?
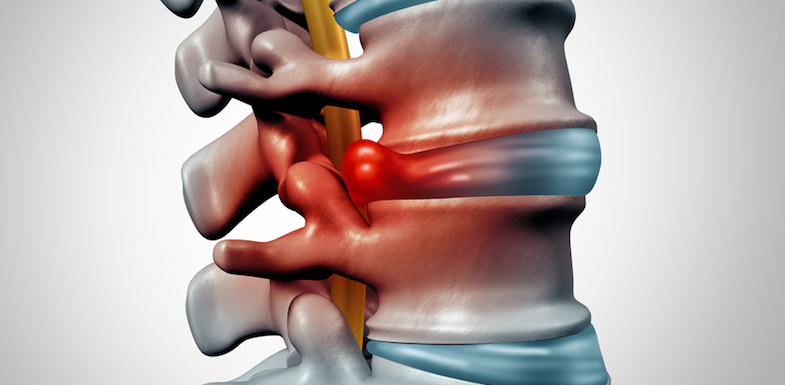
Herniated disc symptoms may vary depending on the individual and where the herniation occurs. Symptoms often come not from the herniated disc itself, but from its contact with your nerves in the spine.
For many people, this means that there are few, if any, early warning signs or symptoms. If your herniated disc has not come into contact with a nerve, then you may not have symptoms at all. In this case, you probably won’t know you have a herniated disc until symptoms manifest, or until a doctor runs tests for another reason and discovers the herniated disc accidentally.
Pain
Once the herniated disc does touch a nerve, you will begin to experience symptoms, including back pain. But pain is not the only symptom associated with disc herniation. You may also experience the following symptoms.
Tingling
Where you feel tingling will depend on where your disc herniation is.
If it’s in your lower back, as is most usual, then you may experience tingling in your leg and foot. If the herniated disc is in your neck, you may feel tingling in your arm and hand instead.
Weakness
With your spine not functioning the way it’s supposed to, you may notice you have more trouble with certain activities, such as walking or bending, than you did before.
Numbness
Some people with a herniated disc lose feeling in certain body parts.
If you have a herniated lumbar disc, then your leg and foot could be affected. If it is a herniated cervical disc, the numbness may affect your arm and hand. A herniated thoracic disc can affect either your upper or lower extremities.
Do I have a herniated disc?
Back pain, especially lower back pain, is incredibly common. Over 80% of adults will experience back pain at some point in their lives, thanks to a wide range of primary conditions. So how can you tell if a herniated disc causes your back pain, or if it’s something else?
By yourself, you can’t, at least not for certain. Only a doctor can make a formal diagnosis, through the use of one or more diagnostic tests.
At your appointment, your doctor will likely perform some basic tests, such as those measuring muscle strength and reflexes. In some cases, your doctor may also take an image of your spine with an X-ray or an MRI. With these images, they can have a direct look at the herniated disc or other problems causing your back pain.
Is a herniated disc serious?
If you have a herniated disc, the prognosis is generally quite good. Symptoms often become less acute over time. In some cases, symptoms go away entirely without treatment. For the majority of patients, herniated disc recovery time is generally a few weeks to a few months.
Knowing this doesn’t make it easier to deal with the pain and other symptoms you have right now, but know that your current situation is generally not permanent and will likely clear up without drastic medical intervention.
Very rarely, a herniated disc becomes serious enough to warrant immediate medical attention. If your symptoms are so severe that you can’t perform basic tasks, go to a doctor or emergency room right away.
Especially serious herniated disc cases may lead to cauda equina syndrome. This rare condition is characterized by extreme lower back pain, weakness and/or numbness in the groin and lower extremities, and loss of bowel and/or bladder control.
If you’re experiencing these symptoms, it requires an emergency trip to the doctor and, in most cases, emergency surgery. Allowing your case to go untreated may result in permanent damage, including incontinence and paralysis.
What are herniated disc treatments?
If your back pain has bothered you for a while, you have probably already sought out ways to treat it on your own. The best way to approach this condition, though, is under your doctor’s care.
Once you receive an official diagnosis, talk with your doctor before starting any new treatments. They’ll discuss treatments that could work best for your exact condition and symptoms, as well as complementary therapies to help with your symptoms.
Rest
Rest is important when you have suffered an injury. But even with this most basic of pain remedies, there is a helpful way and a harmful way to go about doing it.
Long periods of bed rest, for example, can further weaken your back, which will make it even more difficult to recover. Try interspersing periods of rest with periods of gentle exercise, if okayed by your doctor.
Exercise
Some exercises can help you feel better, while others can actually make a herniated disc worse. Walking, for example, is a cheap form of exercise that can often reduce your lower back pain.
Again, talk with your doctor to get an idea of which exercises are best for you. Basically, if an exercise – or any type of movement – aggravates your symptoms, stop. If possible, don’t perform that activity again until your back has healed more.

Lifestyle changes
Losing weight may also relieve herniated disc symptoms and protect your back from similar injuries in the future.
With the guidance and approval of your doctor, you can reach a healthier weight with a low-impact exercise regimen and regular, nutritious meals.
Medications
Many people use medicine to relieve pain. You may already be taking over-the-counter medicines like ibuprofen.
If you are still experiencing significant pain even while taking these medications, talk to your doctor about what could help during acute pain flare-ups.
Physical therapy
Physical therapy is another common herniated disc treatment. A physical therapist is a professional who specializes in helping people regain their previous range of motion as much as possible, while also strengthening the muscles around the injured area.
To do this, they will take stock of your condition and develop a treatment plan specifically for you. This plan will likely include multiple treatment approaches, including exercises, stretches, heat/cold therapy, and more.
Interventional treatments
In some cases, the treatments outlined above will not be enough to manage your pain. If that is true for you, your doctor may suggest a more interventional form of treatment, such as injections or surgery.
Injections, including cortisone injections, can help when your chronic pain becomes too severe to be managed by more conservative treatments. These injections have the potential to offer effective, long-term pain relief, but they can also cause serious side effects if used too frequently. Your doctor will help you decide if the risks are worth the benefits in your case.
There are also multiple kinds of herniated disc surgery, including partial or total removal of the affected disc or the insertion of an artificial disc to replace the damaged one.
Find help for your pain
Only 10% of herniated lumbar discs require surgery. The majority of patients will heal with more conservative treatment approaches and time.
If you live in Arizona and need help with your herniated disc pain, click below to connect with one of the pain specialists at Arizona Pain. Our team can guide you through the treatment process and help select the approach that’s best for you. Together, you’ll develop a treatment plan that combines complementary, non-invasive treatments for longer-term relief, along with interventional approaches if you’re suffering from severe pain.