
The best exercises for sciatica leg pain include stretches that can relieve tightness, yoga poses to reduce tension, and cardio activities like dancing and walking. Learn more about how you can start incorporating these exercises for sciatica leg pain into your daily routine to help you relieve your pain.
Performing exercises for sciatica leg pain
Before getting started on exercises for sciatica leg pain, it’s important to have a really good understanding of what sciatica is and how it’s different from more general types of leg pain or tightness. As some of our presenters of sciatica leg pain exercises will point out, often people believe they have sciatica when it’s actually just tightness in the piriformis muscle.

What is sciatica?
Sciatica is a pain symptom that is felt when the sciatic nerve is irritated or inflamed. Since the sciatic nerve runs all the way down the spinal cord and the legs, the pain follows and may be felt as tingling or numbness in the legs and feet, as well as pain up through the lower back and buttocks. This pain is normally caused by a herniated or slipped disc that impact the sciatic nerve.
Sciatica pain can also be caused by:
- Extreme forms of chronic lower back pain
- Pinched nerves
- Spinal stenosis, a narrowing of the spinal canal that can put pressure on the nerves
- Piriformis syndrome, spasms in the piriformis muscle
- Spondylolisthesis, vertabrae that slip one over the other
Unfortunately, for many people today, sciatica pain can be exacerbated by long bouts of sitting. While there are multiple treatment options, the first preventative step for many office workers is to remain as active as possible during the day and to take short breaks from sitting.
Other simple changes can also have a big impact on sciatica pain, including exercises for sciatica leg pain which we’ll discuss shortly. Other options include proper eating, massages, or physical therapy. Alternative therapies like yoga and acupuncture have also been shown to help people with sciatica pain. People with more advanced sciatica pain may be able to find some relief with non-steroidal anti-inflammatory drugs, like aspirin or ibuprofen, or interventional procedures like epidural steroid injections, Botox injections, spinal cord stimulation, or intrathecal pump implants.
With any form of pain, it’s best to talk with your pain doctor before undergoing any new treatment. This includes exercises for sciatica leg pain. He or she can help you find the best options for your pain symptoms.
You can learn more about sciatica by watching the video below.
What is leg pain?
More general types of leg pain may strike in any part of the lower limb, from the hip to the knee, calf, and on down to the ankle. Causes of leg pain vary greatly, and may be attributed to an acute injury or more serious underlying condition, including sciatica. Types of pain and prognosis vary depending on the cause. As we’ll see, leg pain that occurs in the hips, knees, and ankles are often attributable to other underlying conditions–not sciatica.
Leg pain in the hip
Hip pain is hard to ignore since it can linger and make walking difficult. The hip, formed by a ball-and-socket joint, is built to support our bodies as they run, jump, and walk through life. However, over time, the cartilage that cushions the hip and helps it move smoothly erodes.
This weakened cartilage may lead to arthritis, which causes inflammation and pain. For many people, pain might be the first symptom that arthritis has developed. Pain associated with arthritis feels dull or aching. It may feel worse in the morning and decrease during the day as activity levels increase. Finding a balance in activity may help manage hip pain since vigorous activities like running have been known to exacerbate it, according to the American Academy of Orthopaedic Surgeons (AAOS).
Hip pain may also result from tendinitis, a painful, inflammatory condition typically caused by muscle overuse. Tendons are strong, thick bands of tissue that hold bones and muscles together. Fractures are another potential cause of hip pain, but most frequently occur in elderly people or those with osteoporosis, a condition of thinned bones.
Leg pain in the knee
The knee is the largest joint in the body. It connects the lower leg bones—the tibia and the fibula—with the upper leg bone, or the femur. The knee achieves this monumental task with a network of tendons, ligaments, and muscles. The knee also has a cartilage cap, making this joint also susceptible to the pain of arthritis.
Knees absorb the shock of impact from walking and running, and they frequently break falls while playing sports or just living life. The knee was the joint people most commonly reported as causing pain in a 2006 CDC survey.
While the knee can develop arthritis or other problems resulting in pain, most knee pain is caused by injuries, according to WebMD. Injuries may result from a fall or abnormal twisting of the leg. Parts of the knee susceptible to damage include the meniscus, a tough, rubbery cushion located between the femur and tibia. The tibia is also known as the shinbone. Older people who have weakened cartilage may also tear the meniscus.
Many times, the telltale sign of a meniscus tear is a popping noise. Pain and swelling will continue for several days. Treatment may include rest, ice, and elevation, although surgery is sometimes necessary for more serious tears. The knee may also become swollen or tender from overuse. Tendonitis, strains, and sprains can cause knee pain as they can with other joints in the body.
Leg pain in the ankle
The ankle is a complex cluster of joints and bones that’s responsible for joining the foot to the leg. It bends and turns with an astonishing range of flexibility, but even the mighty ankle succumbs to pain.
A frequent cause of ankle pain is sprain. Sprains may happen from daily activities or from a wrong turn or fall while playing sports or going for a hike. In sprains, the ankle turns or twists in an abnormal direction, resulting in the ligaments sustaining small tears. Symptoms include swelling, bruising, and difficulty walking.
About 40% of people who sprain their ankles develop chronic pain, even after the injury heals, according to a study published in the American Academy of Orthopaedic Surgeons journal. Researchers said these individuals may have torn ankle tendons. Symptoms include pain that doesn’t respond to treatment and pain outside the ankle or behind it.
Arthritis may also develop in the ankle as age wears down the bone and cartilage during daily use. Symptoms of arthritis in the ankle include stiffness, swelling, and difficulty walking. Treatment may include physical therapy, custom shoes, or weight control.
Other causes of leg pain
Other leg pain causes may include:
- Leg cramps: Muscle cramps come on quickly and frequently leave just as fast. Causes may include dehydration or depleted levels of important minerals such as potassium, magnesium, sodium, or calcium. Some medicines, including diuretics or stratins, may cause leg cramps. Another frequent cause is muscle fatigue from overuse or staying in one position for too long.
- Tumors: Although most leg pain is due to injury or arthritis, sometimes leg pain signals a more serious medical condition that requires urgent medical attention. Some bone cancers such as osteosarcoma or Ewing sarcoma result in leg pain. Benign tumors, so called because they’re not cancerous and not fatal, may also grow in the leg and cause pain.
- Blood clots: Blood clots in the legs may also result in pain. Atherosclerosis, the medical term for hardening of the arteries, is the same process that leads to a heart attack, but it can also occur in the leg. Years of fat and cholesterol buildup in the arteries and lead to hard plaque deposits, making it difficult for blood to flow. In addition to pain or discomfort, symptoms include fatigue and achiness.
If you’ve ruled out these leg pain causes and identified sciatica as a source of your pain, it’s time to get started with some exercises for sciatica leg pain.
10 stretches for sciatica leg pain
If your sciatica pain starts from the moment you wake up, try one of these six exercises for sciatica leg pain you can do in bed. Prevention.com shows how to perform each stretch safely and effectively.
If you’re looking for a deeper stretch, try one of the following stretches for sciatica leg pain.
1. Leg up the wall stretch
Dr. Paula Moore gives a quick stretch you can do anywhere in her short video.
2. Low lunge
This classic pose gently stretches the hip flexors. This is a good stretch to help the body relax. Only go so deep into the pose as feels comfortable for you.
- Come to a kneeling position. Send the right leg in front of you, coming into a low runner’s lunge. If the knee feels any strain, fold up a blanket and use it for support.
- Adjust your stance as desired. The lunge can be a long or short one, whichever feels best for you.
- Place the hands on the knee, or if it feels good, lift the arms overhead, breathing into the space behind the heart. Stay here for five to seven breaths, enjoying a gentle opening down the hip flexor and spine.
- Relax and repeat on the other side.
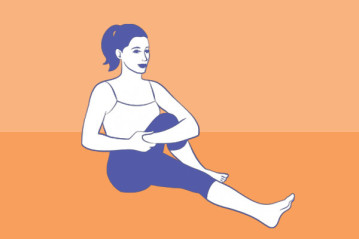
3. Seated hip stretch
This is another classic pose that’s easy to do just about anywhere (even the break room!). Morgan Sutherland at Mind Body Green gives a breakdown and illustration of this sciatica stretch.
4. Foam roller for sciatica pain
This rolling sciatica exercise from Prevention.com is great for opening up the hips and easing pain.
4 yoga poses for sciatica leg pain
When exercises for sciatica leg pain are discussed, yoga is one of the first practices that’s mentioned. And there’s a reason.
People who sit a lot tend to have short, weak hip flexors, so stretching and strengthening helps restore them to better health. Focusing on hip flexor strength and flexibility can help reduce leg and sciatica pain. Yoga does just that. Yoga is a practice of cultivating balance, emphasizing both stretching and strengthening to ensure the muscles become as healthy as possible.

1. Pigeon pose
Healthline.com pulls together multiple examples of how to do this deeply therapeutic pose. Pigeon pose is one of those exercises for sciatica leg pain that can be modified for any person. The most gentle variation is shown below in the GIF Healthline created to illustrate this pose.

2. Extended hand-to-big-toe pose (utthita hasta padangusthasana)
This pose may seem difficult, but it can be modified for any level of ability. It’s excellent for building hip flexor strength, improving balance, and increasing hamstring flexibility.
- Stand tall, with both feet on the ground, hands by your side. Keep the spine nice and long and press all four corners of the feet into the floor.
- Press weight into the left foot, firmly rooting down. Bend the right knee and lift it up towards the stomach, keeping the foot flexed and parallel to the floor. Stay here for a breath.
- If it feels good, clasp your right big toe between your index and middle fingers from the inside of your leg. Begin to straighten the right leg so it’s parallel to the floor. It’s okay to straighten the leg halfway, with a bend still in the knee. Just make sure your back doesn’t hunch forward. Stay as tall as possible.
- If you need to modify this yoga pose for sciatica leg pain, try a strap. Wrap the strap around the ball of the right foot and use it as an extension of your arm. Likewise, an even more gentle variation is to do this pose with a something to rest your foot on, like a tall chair or stool.
- Wherever you are in this posture, keep your shoulders firmly on your back. Find a steady point of focus to help you balance.
- Stay for three to five breaths, simply returning to the posture if you fall out, before repeating on the other side.
3. Boat pose (navasana)
Boat pose is a wonderful strengthener for the entire core. Strengthening the core can help with reducing the tension in your legs. Again, the full pose can be a little intense, but many modifications are available to make this pose suitable for every body.
- Start from a seated position, with your knees bent and feet flat on the floor in front of you. Place your hands on the floor by your sit bone.
- Lift one leg up so the calf is parallel to the ground. The first option is to stay here for a couple of breaths before lowering down and repeating on the other side. Or, if that feels good…
- Lift the second leg up and keep both legs raised simultaneously for about five breaths. Rest and repeat three more times. Leave the hands resting on the floor or extend them straight past the knees. If you’d like a little more…
- Straighten the legs, coming into the full pose, which resembles a V-shape. Keep the spine long with the arms extended straight past the knees. If it feels like too much, don’t be afraid to back out of it and return to the bent-leg version, also known as half-boat, or ardha navasana.
Yoga Journal provides a more in-depth explanation of this yoga pose for sciatica pain.
4. Tiger pose (vyaghrasana)
This gentle movement stretches and strengthens the hip flexors while also strengthening the lower back, making it a highly effective back strengthening exercise for sciatica pain.
- Come to all fours, with the knees underneath the hips and wrists underneath the shoulders. Press firmly down into the finger pads, taking the weight out of the wrist. If the knees hurt, place a rolled-up blanket underneath them for padding.
- Extend your right leg straight behind you. If it’s possible, also extend the left arm in front of you.
- Bend the right leg and bring the knee toward the forehead. If you’re using your arms as well, bring the elbow and knee to touch or as close as possible.
- Maintain the movement, expanding and contracting, in concert with the breath. Continue about five or six times, breathing nice, long, and deep, before switching to the other side.
2 of the best exercises for sciatica leg pain
After you’ve tried stretches and yoga poses for your pain, try out one of these more fun cardio exercises for sciatica leg pain.
1. Dance!
Most of the recommendations to reduce leg and sciatica pain don’t sound very fun, but we’ve got a very special one that’s sure to put a smile on your face and joy in your heart: dancing! That’s right, research has discovered that dancing the night away—or the afternoon for that matter—is a highly effective way to reduce pain and get your groove back. It’s why it’s one of our favorite exercises for sciatica leg pain.
The research behind dancing for leg pain
Researchers at Saint Louis University Medical Center examined senior citizens living in an age-restricted apartment complex. Most residents were women with an average age of 80. All the study participants reported stiffness or pain in their hips or knees, and most of that discomfort was related to arthritis. The specific type of dance used in the program was customized for the needs of people with hip or leg pain.
Researchers noted that dancing was a wonderful way to help seniors become more agile and increase the pace of their walking. Walking speed is important because a gait that’s too slow is considered a risk factor for falling and subsequent injury and hospitalization. Health care professionals consider a person’s walking speed to be a sixth vital sign, researchers said, helping to predict which patients are at high risk for injuries.
But dancing did more than help people walk faster. It also reduced pain and increased quality of life. In the group that danced, people were able to lower the amount of pain medication they took by 39% while people who didn’t dance actually had to increase their pain medicine by 21%. Krampe says:
“Those in the dance group talked about how much they loved it. It’s exercise, but it’s fun… This is not surprising because those in our study are from a generation that loved dancing.”
Dancing is an activity that many younger people do, but with age, those same dance lovers often give it up. But you’re never too old or young to dance. Dancing does more than make you fit and healthy—it makes you smile. In this way, it reduces stress, which can also reduce the amount of pain a person experiences.
Try these types of dancing
If you’d like get into the swing of things, here are some ways to get started.
- Salsa: Salsa is a Latin-themed style of dance, and many classes are held in restaurants and dance centers. Many facilities offer salsa dance socials preceded by lessons, allowing you to learn or fine-tune your skills and then practice and have fun doing the real thing.
- Zumba: Zumba is a popular type of workout that’s infused with Latin-style rhythms. Classes are offered at many gyms. Zumba is also all levels since dancers can move at their own pace and take breaks whenever they’d like to. This is a solo dancing experience, too, making it perfect for those not interested in tangoing with a partner.
- YouTube at home: For a private, no-fear experience, try dancing at home. Let your inhibitions loose and don’t worry about what you look like or even what you’re wearing. YouTube offers many free home workouts that you can try at your own pace, on your own time. From weight loss to cardio dance, YouTube has you covered. Workouts come in a range of lengths, anywhere from ten minutes to 30 and beyond. If you try this option, find a space in your house with hard floors and not carpet. Dancing on carpet can lead to a tweaked knee or ankle since the non-slippery surface inhibits freedom of movement.
- Dancing classes: Dance classes are a bit larger of a commitment because sign-up typically occurs in sessions lasting several weeks. However, lessons are a great way to get out of the house, meet people, and have fun all while dancing and improving your health. Plus, making that commitment could be a good thing, helping you to stick to your newfound hobby long enough to truly decide whether you like it.
2. Walking
Walking is one of the simplest exercises for sciatica leg pain. Even parking the car farther away from your destination or taking a stroll around the block after lunch can provide health benefits, such as as reducing low back pain and lowering the risk of heart disease.

Benefits of walking
One study published in The Lancet found that people who have problems tolerating glucose reduced their risk of heart attack or stroke by walking an additional 2,000 steps per day. That’s about 20 minutes at a moderate pace. The American Heart Association (AHA) considers walking one of the most important things people can do for heart health. The AHA recommends walking for 30 minutes daily, however ten minute walks taken three times a day have the same effect. Every hour of walking helps to increase your life expectancy by two hours, according to the AHA.
Walking also helps to reduce low back pain and sciatica pain. A team of Israeli researchers published a study in Clinical Rehabilitation, revealing that walking two or three times per week for 20 to 40 minutes provides the same amount of lower back relief as specialized physical therapy programs.
Get started
If incorporating 30 minutes of physical activity in your day seems overwhelming, start where you can and progress from there. Incorporating just five minutes of walking into your day helps to create good habits. Once the endorphins from exercise kick in, you might be inspired to move some more!
Tips to get stepping include:
- Wear a pair of comfortable shoes so your feet have adequate support.
- Try to walk at the same time every day, possibly after lunch or dinner, to create a habit.
- Don’t push yourself too hard. If you haven’t exercised for a long time, take it slow and work up to 30 minutes gradually.
- Recruit a walking buddy. Walking with a friend or loved one provides an added push and makes exercise fun.
What other exercises for sciatica leg pain have worked for you? If your sciatica pain isn’t relieved by these exercises for sciatica leg pain, it may be time to talk to a pain doctor. They can provide additional treatment options to relieve your pain.